Psoriatic Arthritis: Managing the Skin and Joint Connection
Psoriatic Arthritis (PsA) is a unique dual-threat condition where the immune system attacks both the skin and the joints. It affects roughly 30% of people who have psoriasis, leading to inflammation that can cause permanent joint damage if left unchecked. In 2026, the focus has shifted toward “disease interception”—catching the condition in its earliest stages to protect joint function and maintain clear skin.
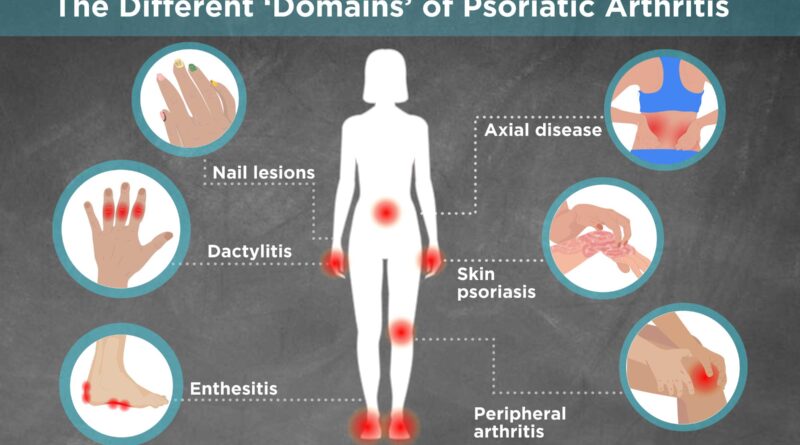
The “Dual-Domain” Impact: Skin and Joints
Unlike other forms of arthritis, PsA is a multi-domain disease. It doesn’t just affect the cartilage inside a joint; it targets the “entheses”—the specific points where tendons and ligaments attach to the bone.
- Dactylitis (Sausage Digits): A hallmark symptom where an entire finger or toe swells uniformly, making it look like a sausage and significantly limiting mobility.
- Reduced Oxygen Exchange: Narrowed arteries mean less blood reaches the air sacs in the lungs. This leads to the The Psoriasis Link: While skin patches often appear first, the severity of the skin rash does not always match the severity of the joint pain. You can have mild skin involvement but aggressive joint inflammation.
- Nail Pitting and Changes: Changes in the fingernails or toenails—such as tiny dents (pitting) or the nail lifting away—are often early warning signs that the joints may soon be affected.
The Rise of Targeted “Oral Small Molecules” and Biologics
In 2026, we have identified three specific biological pathways that control how pulmonary arteries relax and contract. Most moIn 2026, treatment has moved beyond simply masking pain with Ibuprofen. New classes of drugs now target the specific “messengers” in the immune system that cause PsA flares.
- TYK2 Inhibitors: As of March 2026, new oral medications (like deucravacitinib) have been FDA-approved to treat both skin and joint symptoms with a single daily pill, offering an alternative to injections.
- IL-17 and IL-23 Blockers: These “precision biologics” specifically neutralize the proteins responsible for the thick, scaly skin patches and the deep joint inflammation, often leading to near-total skin clearance.
- The “Treat-to-Target” Strategy: Rheumatologists now use a “Targeted Approach,” adjusting medications frequently until a state of “Minimal Disease Activity” (MDA) is reached, rather than just waiting for symptoms to get worse.
Lifestyle Anchors and Joint Protection
Because PsA is an inflammatory condition, lifestyle choices can either “fan the flames” or help dampen the immune system’s overactivity.
- The Impact of Weight: Fat tissue produces inflammatory chemicals called cytokines. Studies show that losing even 10% of body weight can significantly improve how well PsA medications work.
- Low-Impact Movement: Activities like swimming, cycling, and yoga keep joints lubricated and flexible without the “pounding” of high-impact sports, which can trigger enthesitis (tendon inflammation).
- Smoking Cessation: Smoking is a major trigger for PsA flares and has been clinically proven to make certain biologic treatments less effective. Quitting is considered a core part of the medical treatment plan.
Final Thoughts
Psoriatic Arthritis is a progressive condition, but it is no longer a guaranteed path to disability. With the arrival of highly selective oral treatments and a better understanding of the skin-joint connection in 2026, the goal is now remission. If you have psoriasis and start to feel “stiff” in the morning or notice swelling in your toes, early intervention can be the difference between permanent damage and a lifetime of active movement.